
Greetings Acumen blog readers! I hope this note finds you safe and well in the midst of the chaos that surrounds us these days. I am a few days late with a Halloween-related post, but rest assured I will keep a promise I made many years ago and stay away from politics in this forum (try saying that with 280 characters!). While creating this post, I was struck by the fact that our first Acumen blog post hit the blogosphere in September of 2010. And while a decade is certainly a long time, our topic today has a much longer history. So, before the treats you acquired during a Halloween where masks had new meaning become stale, let’s unwrap a remarkable opportunity for patients with ESRD.
Medicare Advantage
As some may not be familiar with its storied past, Medicare Advantage (MA) has been around for over 20 years. MA emerged from a law Congress established in the late 90s that authorized CMS to contract with public and private payors to create additional health care insurance options for Medicare beneficiaries. After a slow start, enrollment in MA began a very steady climb as noted in this bar chart from the Kaiser Family Foundation.
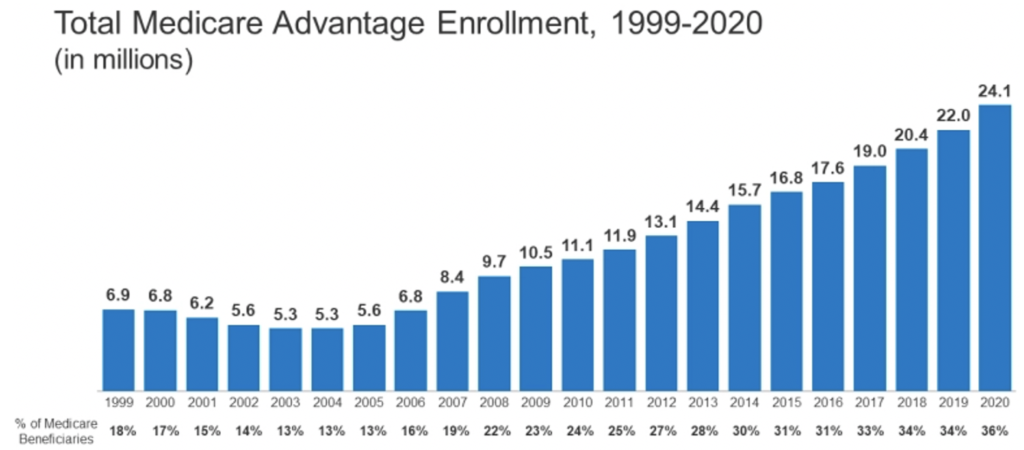
As noted above, approximately 36% of the Medicare population elected to enroll in a MA plan for calendar year 2020.
Why the popularity? Great question. MA plans offer a number of things that are not readily available within traditional Medicare. For example, with traditional Medicare, there is no limit to the patient’s out-of-pocket expense. As you may recall, Medicare covers 80% of the “allowable.” The patient is responsible for the other 20% (often referred to as cost sharing). With MA, the patient’s out-of-pocket expense is capped, and in many MA plans, it is substantially reduced. MA plans also offer several supplemental benefits, like dental care, eye exams, and fitness memberships.
Unfortunately, until very recently ESRD patients covered by traditional Medicare have been excluded from enrolling in general Medicare Advantage plans. However, that exclusion from Medicare Advantage has now changed.
21st Century Cures Act
A piece of legislation known as the 21st Century Cures Act has removed the MA exclusion for dialysis patients. For the first time in history, every ESRD patient covered by traditional Medicare may enroll in a Medicare Advantage plan during what’s known as the Open Enrollment period.
Open Enrollment
What in the world is Open Enrollment? Medicare recognizes that the benefits offered by MA plans can change every year. Fees can change, provider networks can change, medication tiers in prescription drug plans can change. In order to permit Medicare beneficiaries to select the best health plan for their specific circumstances, every year between October 15 and December 7, Medicare beneficiaries can examine their options and move to a new plan if they wish. If a patient elects to change coverage, the new plan assumes coverage of their healthcare on January 1 of the following year. For the first time since the establishment of Medicare Advantage, during this year’s Open Enrollment period, our dialysis patients covered by traditional Medicare can enroll in an MA plan, with coverage beginning January 1, 2021.
Trick or treat?
This is a tremendous opportunity for patients with ESRD, but it is also a daunting opportunity. The number of plans available can vary substantially based on where the patient lives. As we all know, our patients see a number of physicians and take a large number of medications. Getting this right is very important. Add to this the fact that Medicare has some very bright lines around who can discuss Medicare Advantage options with patients (you and I cannot), and it becomes extremely important to ensure our patients have that conversation with an insurance broker.
Call to action
If we are not permitted to speak to patients about specific MA plans, what can we do? Well, we could wipe our hands of this matter and stick our heads in the sand, letting our patients navigate the morass on their own. But as a nephrologist reminded me last week, simply ignoring this opportunity for our patients is doing them a disservice. What we can and should do is make sure our patients know they have the option to enroll in Medicare Advantage. That can start by pointing them to patient-facing sources of information like this one.
Many insurance brokers have little to no experience with ESRD. Our patients are seeing ads on television and receiving cold calls from brokers. This can be a very confusing time for our patients. Ensuring they know there are brokers out there who understand the complexities of their disease state is very important. While switching to an MA plan may not be the best option for some patients, there are many ESRD patients who would be better off in MA. We owe them the opportunity to learn about this from reliable sources. This is time sensitive as the window of opportunity closes in 34 days.
Open Enrollment can be tricky, but this is a wonderful treat for many of our patients. We need to make sure they are aware of this important opportunity.
What are your thoughts about this provision of the Cures Act? Send us a comment and let us know how you are approaching this opportunity for your patients with ESRD.
 Terry Ketchersid, MD, MBA, practiced nephrology for 15 years before spending the past seven years at Acumen focused on the Health IT needs of nephrologists. He currently holds the position of Chief Medical Officer for the Integrated Care Group at Fresenius Medical Care North America where he leverages his passion for Health IT to problem solve the coordination of care for the complex patient population served by the enterprise.
Terry Ketchersid, MD, MBA, practiced nephrology for 15 years before spending the past seven years at Acumen focused on the Health IT needs of nephrologists. He currently holds the position of Chief Medical Officer for the Integrated Care Group at Fresenius Medical Care North America where he leverages his passion for Health IT to problem solve the coordination of care for the complex patient population served by the enterprise.
Image from canstockphoto.com.



Leave a Reply